There are no entries matching your search criteria.
A
Acute wound: A disruption in the integrity of the skin and underlying tissue that progress through the healing process in timely and uncomplicated manner
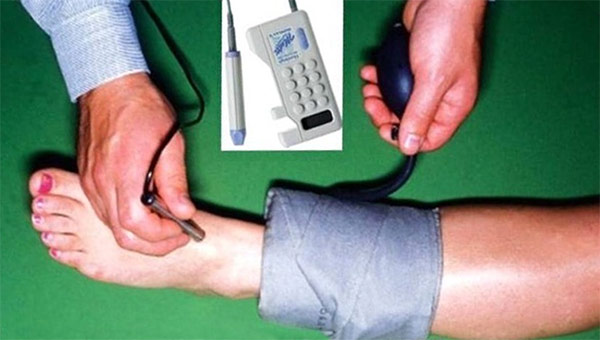
Ankle-Brachial Index (ABI): Comparison of perfusion pressures in the lower leg with those in the upper arm using a blood pressure cuff and handheld Doppler ultrasound device. Diagnostic tools for detecting lower extremity arterial disease (LEAD). Can be performed by trained professionals at the bedside.
Autologous skin graft: Graft of patients own skin, autograft
Autolysis: When the body’s own leukocytes and enzymes break down or liquefy tissue or cells. Happens with autolytic debridement.
B
Bioburden: Presence of microorganisms on or in a wound. Continuum of bioburden ranges from contamination, colonization, critical colonization, biofilm and infection. Bioburden includes quantity of microorganisms, their diversity, virulence, and interactions with each other and the body
Biofilm: Polysaccharide matrix that microorganisms produce and live in. Group of microorganisms very resistant and poorly penetrated by antimicrobials. Only removable by debridement. Its presence in a wound can be a precursor to infection
C
Clean wound: Wound free of dead tissue, purulent drainage, debris or foreign materials
Closed wound edges: (epibole, hyperkaratotic) When top layer of epidermis rolls down and covers bottom layer of epidermis, epithelial cells no longer can move across wound bed. Presents as a hardened or discolored sealed wound edge
Chronic wound: Wound that deviates from expected sequence of repair in terms of time, appearance, and response to aggressive and appropriate treatment
Collagen: Main supportive tissue of skin, tendon, bone, cartilage and connective tissue
Colonization: Replicating of microorganisms on the wound bed without host reaction
Critical Colonization: Replicating of microorganisms present on the wound and attaching to the cells and structures in the wound
Crusted: Dried secretions
D
Dead space: Deficit or cavity
Debridement: removal of dead tissue
Denude: Loss of epidermis
E
Epithelialization: Regeneration of epidermis across a wound surface
Eschar: Black or brown necrotic tissue that can be loosely or firmly adherent, hard or soft, dry or wet
Excoriation: Linear scratches on the skin
Exudate: Accumulation of fluid in a wound. May contain serum, cellular debris, bacteria and leukocytes
F
Fibroblast: Cell from which connective tissue is developed
Full thickness: Tissue damage involving total loss of both the epidermal and dermal layers extending into the subcutaneous layer, possibly into the muscle or bone
G
Granulation: Formation or growth of small blood vessels and connective tissue in a full thickness wound
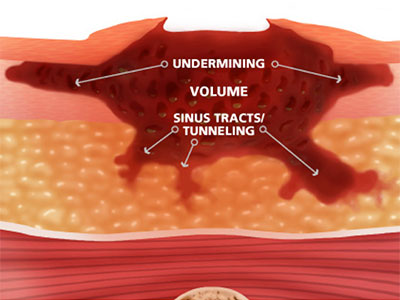
Granulation tissue: Pink/red, moist tissue composed of new blood vessels, connective tissue, fibroblasts, and inflammatory cells, which fills an open wound as it is healing. Deep pink/red with berry like or cobblestone appearance
Growth factors: Polypeptides that control growth and differentiation of cells
H
Hypergranulation: Excess granulation tissue extended above the level of the skin. Epithelial cells unable to migrate up and over this tissue
Hyperkeratosis: Hard, white/gray tissue surrounding a wound
Hypertrophic:
I
Induration: Abnormal firmness of tissue with a definite margin, usually indicated infection
Insulation: Maintenance of wound temperature close to body temperature
J (no entries)
K (no entries)
L (no entries)
M
Maceration: Softening of tissue caused by soaking in fluid
MMP: Matrix metalloproteinase; enzymatic compound capable of protein and connective tissue degradation. Excess MMPs may impede healing
N
Newly epithelialized: Process of regeneration of epidermis across wound surface
Nonepithelialized: Absence of regenerated epidermis across wound surface
Nongranulating: Absence of granulation tissue, wound surface appears pink and smooth as opposed to granular. Wound has no slough/eschar but also has no granulation tissue. Can be referred to as “stalled” wound
Nonviable: Non-living tissue (slough or eschar)
O
Occlusive wound dressing: No liquids or gasses can be transmitted through the dressing material
P
Partial thickness: Confined to the skin layers. Damage does not extend below into the dermal layer
Periwound: Area immediately surrounding the wound
Primary Dressing: Therapeutic or protective covering applied directly to the wound bed to meet the needs of the wound
Purpura: Bleeding beneath the skin or mucous membranes; causes black and blue spots or pinpoint bleeding
Q (no entries)
R (no entries)
S
Scab: A crust of dried blood and serum
Secondary dressing: Therapeutic or protective function and is used to increase the ability to adequately meet the wound needs and/or secure the primary dressing
Semiocclusive wound dressings: No liquids are transmitted through dressing, variable levels of gases can be transmitted through dressing. Most dressings are semiocclusive
Slough: Soft, moist, avascular tissue that can be white, yellow, tan, gray. Can be loosely or firmly adherent
T
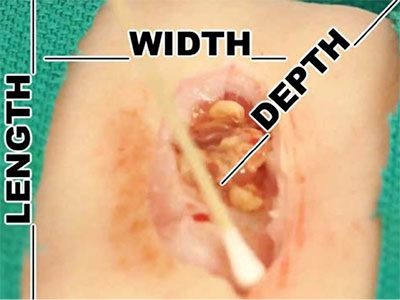
Tunneling: Course or path of tissue destruction occurring in any direction from the surface or edge of the wound, results in dead space, potential for abcess formation (also referred to as sinus tract)
U
Undermining: Area of tissue destruction extending under intact skin along the periphery of the wound. Can be distinguished from tunneling in that undermining involves a significant portion of the wound edge, whereas tunneling only involves a small portion
Unstageable pressure ulcer: Covered with eschar or slough, which prohibits complete assessment of the wound
V (no entries)
W
Wound margin/edge: Rim or border of the wound
X
Xenograft: Tissue from another species used as a temporary graft