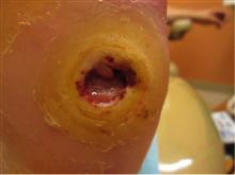
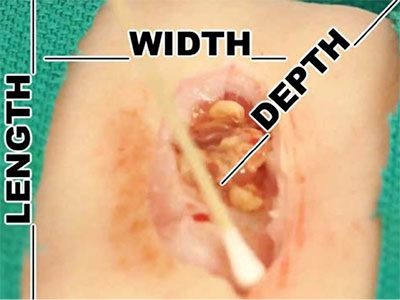
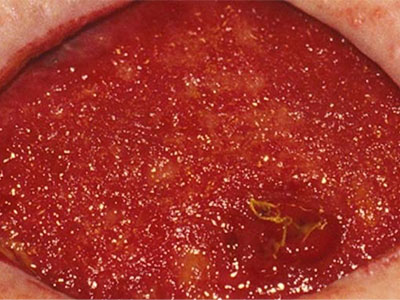
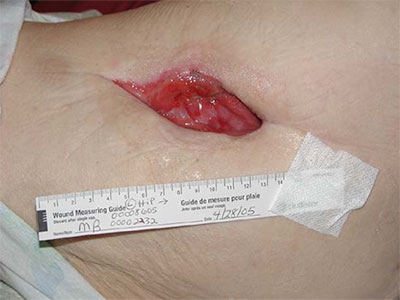
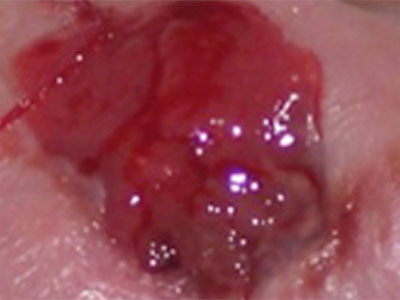
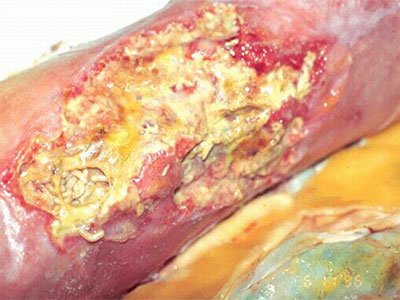
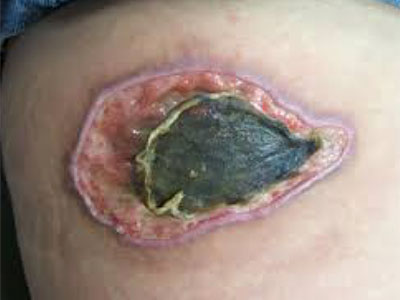
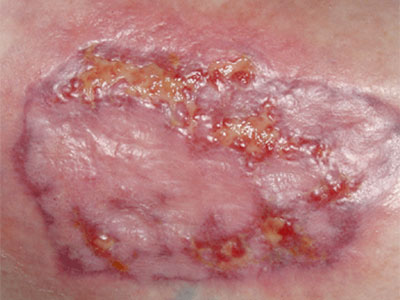
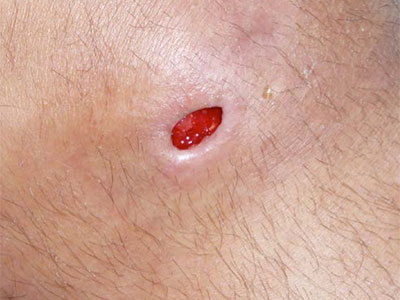
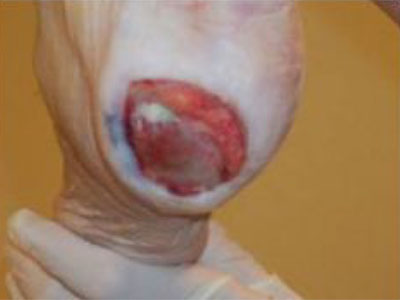
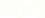Clinical Pathways for the 5 Wound Types
Choose a wound type to view the associated clinical pathways and guidelines.
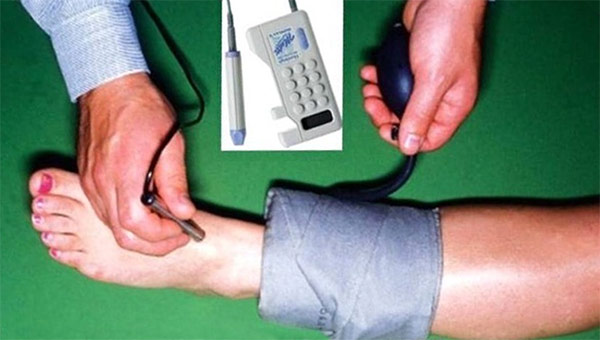
Diabetic Ulcer Pathway
References
Glycemic control and post-operative healing. Journal of Foot and Ankle Research; Lower Extremity Review. Naohiro Shibuya, DPM, MS, FACFAS, Jon M. Humphers, DPM, and Daniel C. Jupiter, PhD. July 2013
>Guidelines for the treatment of diabetic ulcers; Wound Repair and Regeneration (2006). Wound Healing Society. Steed, David
Diagnosis and treatment of peripheral arterial disease in diabetic patients with a foot ulcer. A progress report of the International Working Group on the Diabetic Foot. Diabetic foot infection: Antibiotic guidelines. Johns Hopkins. Eric Nuermberger. 6/16/2009
Lipsky BA, Berendt AR, Deery HG, et al.; Diagnosis and treatment of diabetic foot infections.; Clin Infect Dis; 2004; Vol. 39; pp 885-910; ISSN: 1537-6591; PUBMED 15472838
Debridement: A Vital Component of Wound Bed Preparation. Kirshen C, Ayello E, Sibbald, R. Advances in Skin Wound Care 2006; 19:506-17; Lippincott Williams & Wilkins.